Dr. Hamad Husainy on AI in Emergency Medicine: Restoring Clinical Clarity in a Data-Saturated ED
AI restores clinical clarity in data-saturated EDs through workflow-embedded insight.

.png)
The Information Crisis Inside the Emergency Department
Emergency departments (EDs) have always operated at the edge of chaos. But over the past decade—and especially post-COVID—the structural pressures have intensified: rising patient volumes, staffing shortages, higher acuity, and a growing proportion of patients with behavioral health and social complexity.
In this environment, the core problem is no longer data scarcity. It is data saturation without context.
According to Dr. Hamad Husainy, practicing emergency physician and Chief Medical Officer at PointClickCare, clinicians are “inundated with data, very little of which is helpful at that moment.” The modern ED is a paradox: enormous information availability trapped inside fragmented electronic health records (EHRs), faxes, paper packets, and siloed systems.
The promise of AI in Emergency Medicine is not to generate more data—but to transform overwhelming information into actionable clinical insight at the bedside.
LLMs as Clinical Co-Pilots (Not Decision Makers). Read more here!
Glossary of Key Terms:
Electronic Health Record (EHR). An Electronic Health Record (EHR) is a digital version of a patient’s medical history that integrates clinical data, documentation, medications, imaging, and laboratory results across care settings.
Natural Language Processing (NLP). Natural Language Processing (NLP) is an AI technique that enables computers to extract structured, clinically meaningful information from unstructured medical text such as physician notes.
Predictive AI. Predictive AI refers to machine learning systems that analyze large volumes of clinical data to forecast outcomes such as readmission risk in real time.
Value-Based Care. Value-Based Care is a healthcare reimbursement model that rewards providers based on patient outcomes, quality metrics, and cost efficiency rather than service volume.
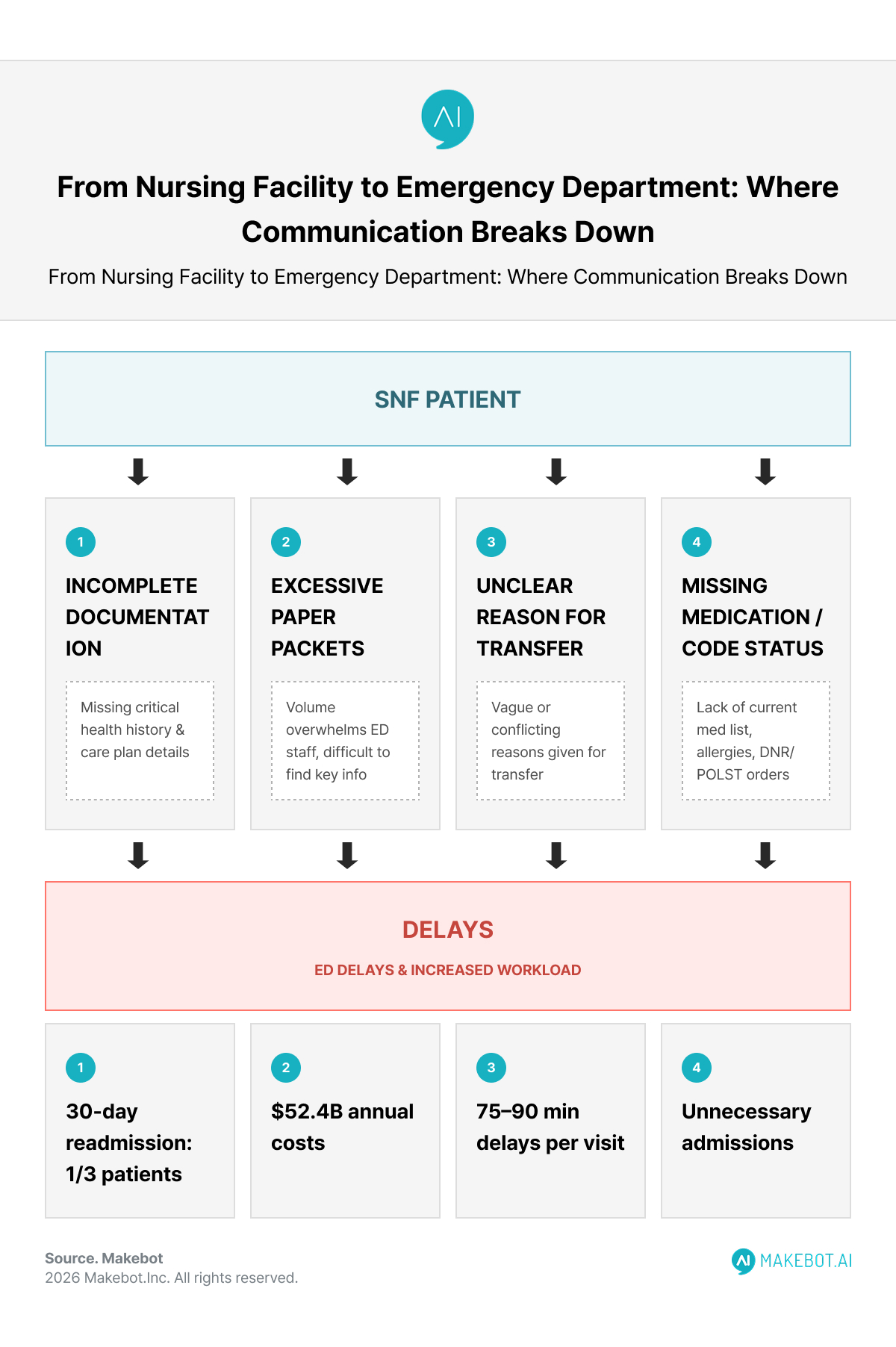
The Post-Acute Transfer Problem: A Structural Weakness in Emergency Care
One of the most operationally fragile moments in acute care occurs when a patient is transferred from a skilled nursing facility (SNF) to the ED.
These patients frequently arrive:
- With incomplete documentation
- With excessive, unstructured paper packets
- Without a clear “reason for transfer”
- Without up-to-date medication or code status details
The consequences are measurable:
- One-third of patients discharged to SNFs return to the ED within 30 days
- These avoidable readmissions contribute to $52.4 billion in annual costs
- Duplicative diagnostics (e.g., repeated CT scans) add 75–90 minutes per visit
- Delayed context leads to unnecessary admissions
This is precisely the inefficiency AI in healthcare is designed to target.
The “Reason for Transfer” Model: Applied Medical AI in Practice
At PointClickCare, Dr. Hamad Husainy and his team developed the Reason for Transfer AI Model—a practical example of Medical AI embedded directly into ED workflows.
Architecture Overview
The system:
- Ingests SNF EHR notes in real time
- Applies natural language processing (NLP) to extract clinically relevant changes
- Summarizes events from the prior 24 hours
- Pushes structured insights into the ED clinician’s EHR interface
The emphasis is critical: pushed intelligence, not passive search.
Rather than forcing physicians to navigate multiple systems during hour 7 of a shift—when cognitive fatigue peaks—the model delivers:
- Vital sign changes
- Medication adjustments
- Adverse reactions
- Fall incidents
- Stroke indicators
- Treatment modifications
Within seconds of patient arrival.
The full documentation remains accessible for validation—an essential safeguard for responsible AI Development—but the summary accelerates triage and decision-making.
From Information Retrieval to Clinical Decision Acceleration
Emergency medicine operates on compression of time. Decisions that might unfold over days in primary care must be made within minutes.
Here is where AI Innovation becomes operationally meaningful.
Example: Reducing Duplicative Imaging
If an ED physician does not know a patient had a negative CT scan 24 hours prior, they are likely to repeat imaging “just in case.” With AI-powered summaries:
- Prior imaging is surfaced immediately
- Clinicians can confidently avoid unnecessary radiation
- ED dwell time drops
- Throughput improves
The impact compounds at scale.
Key Healthcare AI Trends Shaping Innovation in 2026. Read here!
Predictive AI vs. Traditional Risk Scoring
Beyond summarization, Husainy highlights the use of machine learning models trained on millions of SNF residents to predict readmission risk.
These models reportedly outperform LACE (Length of stay, Acuity, Comorbidities, ED visits)—a gold-standard human-derived index—by nearly 30%.
Why?
Because machine learning models:
- Process vastly more variables
- Update continuously
- Identify nonlinear relationships
- Generate evidence-based risk scores in real time
This is a transition from descriptive analytics to predictive AI in healthcare—and it changes how emergency departments allocate resources.
High-risk patients can receive:
- Earlier case management involvement
- Targeted care pathways
- Proactive discharge planning
The result: fewer preventable readmissions and improved value-based care metrics.
Real-World Impact: Sutter Health Case Study
Sutter Health, operating 23 emergency departments in California, provides one of the clearest operational examples.
Through ED Optimization tools:
- Readmissions reduced from 3.4 days to 1.9 days
- Length of stay dropped from 27 hours to 2–3 hours in certain high-utilizer cases
- Behavioral health interventions triggered earlier
- Frequent ED users (200–300 visits/year in some cases) identified instantly
Emergency physicians are interrupted roughly 19 times per hour. Under these cognitive conditions, requiring manual data retrieval is unrealistic. AI-driven summarization improves not only efficiency but clinician morale.
As Husainy notes, “Our biggest asset as a clinician is actually our time.”
Beyond Efficiency: Safety and Risk Mitigation
The benefits extend beyond speed.
1. Code Status and Medication Risk
Real-time insight prevents:
- Inappropriate thrombolytics in patients on anticoagulants
- Unwanted resuscitation in patients with DNR status
2. Behavioral Health Alerts
Early identification of:
- Prior violence risk
- Opioid use disorder
- Mental health crises
Enables:
- Case manager activation
- Safer staff preparation
- Appropriate care redirection
3. Reduced Unnecessary Admissions
Hospitalization itself carries morbidity risk. Avoiding preventable admissions protects patients and reduces cost burden.
Generative AI vs. Workflow-Embedded AI
While Generative AI often dominates headlines—physician note drafting, conversational interfaces—the more transformative impact in emergency care may come from:
- Targeted NLP summarization
- Risk prediction models
- Context-aware alerts
- EHR-agnostic interoperability layers
Generative systems excel at language synthesis. But in high-acuity emergency workflows, structured intelligence delivered at the right moment often produces greater ROI.
The lesson from Dr. Hamad Husainy is that adoption hinges on workflow alignment—not novelty.
Value-Based Care Alignment
AI-driven reduction of:
- Duplicative diagnostics
- Preventable admissions
- Unnecessary transfers
- Extended ED boarding
Directly supports value-based reimbursement models.
As payers expand readmission penalties and quality benchmarks, AI-supported ED operations become not just clinically beneficial—but financially strategic.
Responsible AI: Trust as a Clinical Requirement
Husainy repeatedly emphasizes responsible AI Development. For Medical AI to succeed in emergency medicine, it must:
- Preserve clinician authority
- Provide traceability to source documentation
- Perform equitably across patient populations
- Protect patient privacy
- Avoid automation bias
In high-stakes environments, opacity erodes trust. Transparent systems accelerate adoption.
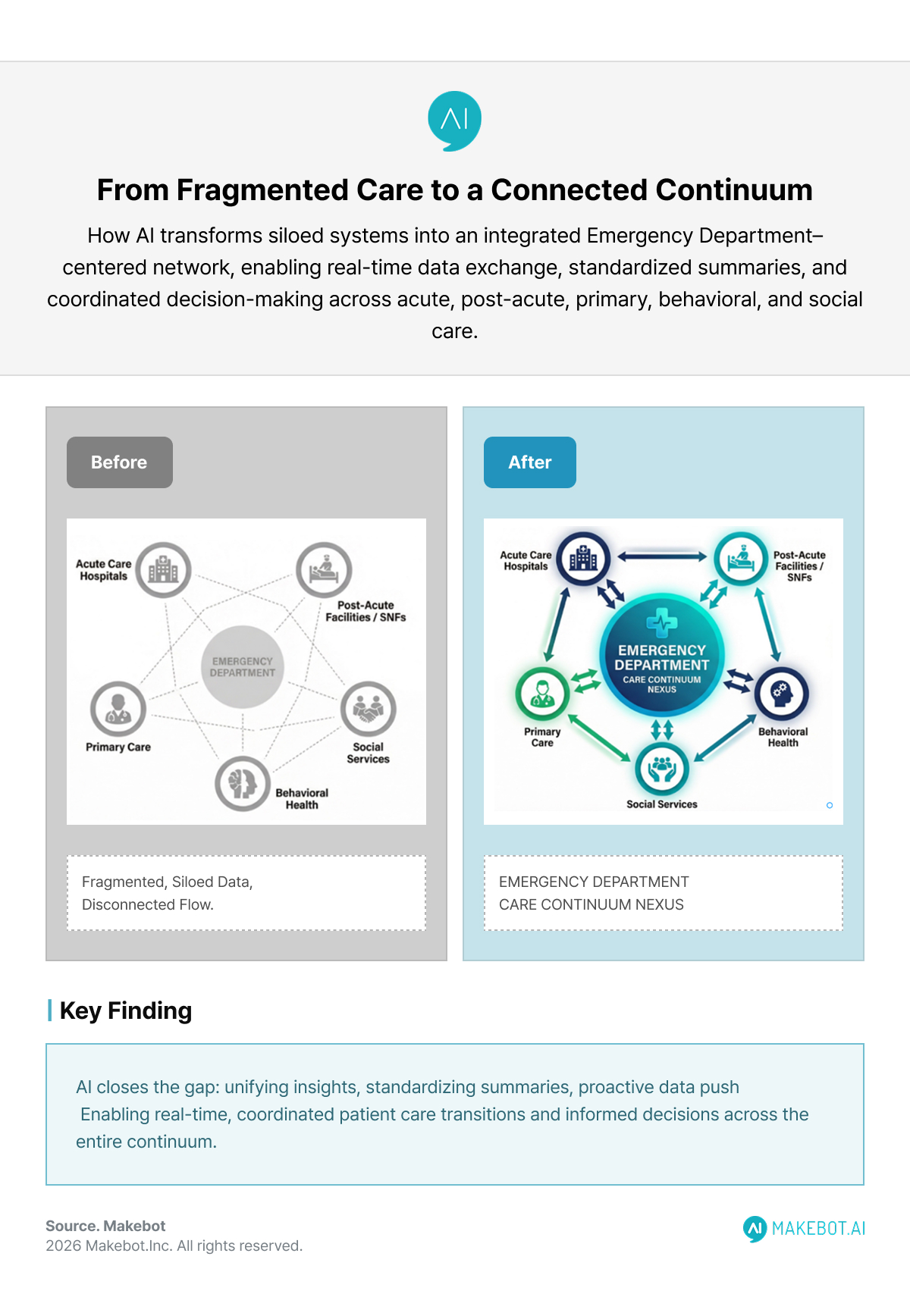
The ED as the Nexus of the Care Continuum
Emergency departments increasingly function as the central hub between:
- Acute care
- Post-acute facilities
- Primary care
- Behavioral health
- Social services
Historically, information fragmentation created a “black hole” during transitions.
AI closes that gap by:
- Unifying cross-setting insights
- Standardizing summaries
- Proactively pushing data
- Supporting bilateral communication
This repositions the ED from episodic crisis center to coordinated care orchestrator.
The Strategic Takeaway
The story of AI in Emergency Medicine is not about replacing physicians. It is about restoring clinical clarity.
From reducing unnecessary CT scans to preventing avoidable readmissions, from improving ED throughput to enhancing staff morale, the implementation described by Dr. Hamad Husainy demonstrates a pragmatic blueprint:
- Integrate AI directly into workflows
- Push concise, actionable summaries
- Validate outputs transparently
- Align models with value-based incentives
- Start with high-friction transition points
Emergency medicine will always be high-pressure. But the intelligent application of AI in healthcare offers a path toward faster, safer, and more coordinated care—without adding cognitive burden.
The future of emergency care will not be defined by more data.
It will be defined by better context, delivered at the right moment, in the right format.
And that is where thoughtful AI Innovation makes its most profound impact.
Applying AI in Emergency Medicine—From Insight to Action
High-quality, cross-continuum clinical data
Seamless ED workflow integration
Transparent, traceable AI governance
The future of AI in Emergency Medicine will not be fully human-driven nor fully algorithm-driven. It will be hybrid—where clinicians, structured data, and Generative AI collaborate in real time.
Faster triage. Smarter transfers. Safer dispositions.
Showcasing Korea’s AI Innovation: Makebot’s HybridRAG Framework Presented at SIGIR 2025 in Italy. Read here!
At this intersection, Makebot bridges research and real-world deployment. We enable the practical implementation of AI in healthcare through:
- HybridRAG-based clinical knowledge architecture optimized for speed and precision
- Workflow-embedded AI systems compatible with existing hospital EHR environments
- Explainable AI frameworks supporting clinician oversight
- Cost-efficient large-scale document intelligence for high-stakes environments
Through production-ready LLM agents and proven HybridRAG infrastructure, Makebot supports healthcare organizations moving from experimentation to operational Medical AI deployment.
Considering how to implement responsible, scalable AI Innovation in your clinical environment?
👉 Start your AI transformation: www.makebot.ai
📩 Inquiries: b2b@makebot.ai

Why Generative AI Projects Fail and How to Achieve Scalable AI Success






















.jpg)





















































_2.png)

















.jpg)


