How Generative AI and Automation Are Transforming Nursing Burnout Across Modern Healthcare Systems
GenAI reduces nursing burnout by shifting clinical workflows from task overload to augmentation.


Primary Keywords : Generative AI , AI in healthcare , nursing burnout solutions , automation in healthcare , healthcare workforce burnout , AI for nurses , digital health transformation , clinical workflow automation , healthcare AI solutions , nurse workload reduction technology healthcare staff retention strategies
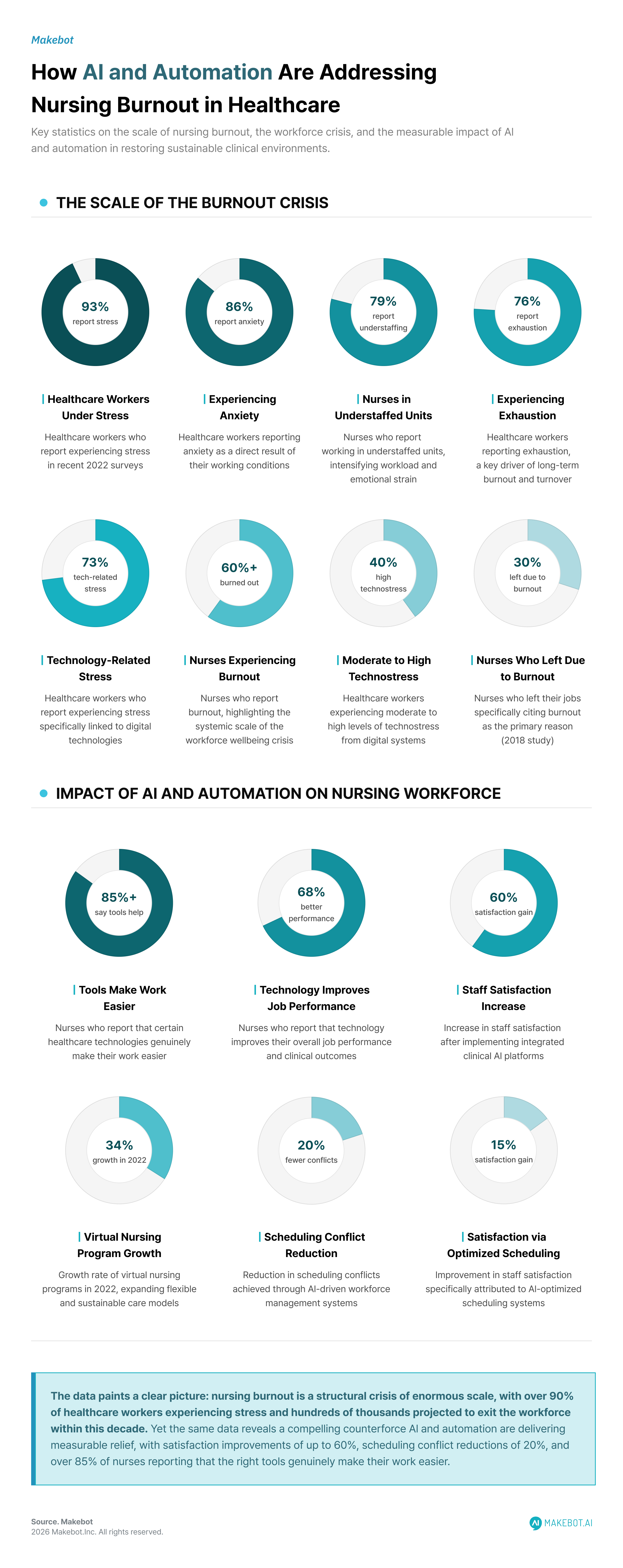
The global healthcare system is facing a structural workforce crisis, with healthcare workforce burnout emerging as one of its most urgent and costly challenges. Even before the pandemic, burnout had already begun eroding nurse retention and care quality. A 2018 study found that 30% of nurses left their jobs due to burnout, while more recent 2022 surveys show that 93% of healthcare workers report stress, 86% anxiety, and 76% exhaustion .
The implications are systemic. High turnover—According to the NSI National Health Care Retention and Staffing Survey, the average cost to recruit new nurses exceeds $50,000 and can take upwards of 85 days—creates compounding operational strain . At the same time, projections indicate that 900,000 nurses may leave the workforce by 2027, while 4.7 million could retire by 2030, intensifying shortages globally .
Against this backdrop, AI in healthcare, automation, and digital infrastructure are not merely tools of efficiency—they are becoming foundational to workforce sustainability. However, their impact is neither uniformly positive nor straightforward. The transformation of nursing burnout is defined by a critical tension: technology as both a stress amplifier and a systemic solution.
McKinsey: AI Could Save the Healthcare Industry $360 Billion Annually. Read more here!
The Root Causes of Nursing Burnout: Beyond Workload
Burnout is not simply the result of long hours—it is the outcome of structural inefficiencies embedded in clinical workflows.
Nurses spend approximately one-third of their shift on routine administrative tasks, including documentation, medication management, and supply retrieval . These repetitive processes reduce time for direct patient care while increasing cognitive fatigue. Simultaneously, 79% of nurses report understaffed units, exacerbating workload intensity and emotional strain .
This is where clinical workflow automation and nurse workload reduction technology begin to play a transformative role—not by replacing clinical expertise, but by redistributing effort away from low-value tasks.
Automation in Healthcare: Redesigning Clinical Workflows
From Task Saturation to Task Delegation
The most immediate impact of automation in healthcare lies in its ability to eliminate repetitive, time-consuming processes. Technologies such as Electronic Health Records (EHRs), Electronic Medication Management Systems (EMMS), and robotic assistants are fundamentally reshaping how nursing work is structured.
- Nurses can now access real-time patient data through EHRs, reducing documentation errors and improving coordination.
- EMMS reduces medication errors caused by illegible handwriting or incorrect dosing.
- Robotic systems handle logistics tasks such as transporting supplies and medications, reducing physical strain.
These innovations are not marginal gains. Studies show that 68% of nurses report that technology improves their job performance, while more than 85% say certain tools make their work easier .
More importantly, automation directly targets burnout drivers:
- Reducing repetitive tasks
- Minimizing administrative overload
- Improving workflow predictability
This aligns closely with emerging nursing burnout solutions, where operational redesign—not just wellness programs—is the central strategy.
The Rise of Generative AI and Intelligent Clinical Support
While automation addresses task execution, Generative AI represents a deeper shift: augmenting cognitive workflows.
AI as a Clinical Co-Pilot
Modern healthcare AI solutions extend beyond rule-based systems into adaptive, data-driven intelligence. Key applications include:
- Automated documentation: AI systems generate clinical notes from interactions, significantly reducing charting time.
- Clinical decision support systems (CDSS): AI analyzes large datasets to provide real-time, evidence-based recommendations.
- Predictive analytics: AI forecasts patient deterioration and workload surges, enabling proactive interventions.
- Virtual nursing assistants: Tools like AI-powered assistants surface relevant patient data within EHR systems.
These capabilities directly address one of the most critical burnout drivers: cognitive overload.
For example, AI-enabled documentation reduces the administrative burden that the American Nurses Association identifies as a key contributor to burnout, where nurses risk becoming “data entry clerks” rather than clinical decision-makers .
Similarly, predictive analytics enables nurse workload reduction technology by identifying bottlenecks before they escalate into crises.
The Growing Role of AI Chatbots in Modern Healthcare Communication. Read here!
Digital Health Transformation and Workforce Sustainability
The integration of AI and automation is part of a broader digital health transformation that is redefining care delivery models.
Virtual Nursing and Telehealth Expansion
Telehealth adoption accelerated dramatically during COVID-19, with virtual nursing programs growing by 34% in 2022 . These models redistribute workload by enabling:
- Remote patient monitoring
- Virtual consultations
- Decentralized care delivery
This shift has measurable workforce benefits:
- Reduced physical strain
- Increased scheduling flexibility
- Extended career longevity for older nurses (average age: 52)
At the same time, telehealth improves access for underserved populations, aligning operational efficiency with equity outcomes.
Measurable Impact: Burnout Reduction and Staff Retention
The effectiveness of AI for nurses and automation is increasingly supported by empirical data:
- 60% increase in staff satisfaction after implementing integrated clinical platforms
- 20% reduction in scheduling conflicts using AI-driven workforce management systems
- 15% improvement in staff satisfaction through optimized scheduling
- More than 60% of nurses report burnout, highlighting the scale of the problem these tools address
From a financial perspective, reducing turnover through healthcare staff retention strategies delivers significant ROI, given the high cost of recruitment and onboarding.
The Double-Edged Nature of Technology
Despite its potential, technology is not inherently a solution. Poor implementation can exacerbate burnout.
The Usability Problem
A 2020 study linked low usability systems to increased burnout, highlighting that fragmented or poorly integrated tools create friction rather than efficiency .
Nurses frequently report frustration with:
- Multiple unintegrated platforms
- Complex interfaces
- Workflow disruptions during system transitions
Additionally, 73% of healthcare workers report technology-related stress, with 40% experiencing moderate to high levels of technostress . This reinforces a critical insight: technology design—not just adoption—determines outcomes.
Reducing Hallucinations in Clinical LLMs Using Retrieval Augmented Generation. Read here!
Ethical, Operational, and Human Limitations
The expansion of AI in healthcare introduces non-trivial risks that must be addressed.
1. Ethical and Data Governance Challenges
- AI systems rely on sensitive patient data, raising privacy concerns
- Algorithmic bias may reinforce healthcare disparities
- Regulatory compliance (e.g., HIPAA) becomes more complex with AI integration
2. Workforce Adaptation Barriers
- Learning curves can temporarily increase workload
- Lack of training is a major barrier to adoption
- Technological overwhelm contributes to emotional exhaustion
3. Risk of Over-Automation
AI must remain augmentative, not substitutive. Clinical judgment, empathy, and patient interaction cannot be automated without compromising care quality.
Strategic Implications for Healthcare Leaders
To fully realize the benefits of healthcare AI solutions, organizations must move beyond tool adoption toward system-level transformation.
Key Priorities:
- Human-Centered Design
- Prioritize usability and workflow integration
- Co-develop solutions with frontline nurses
- Integrated Technology Ecosystems
- Eliminate fragmented systems
- Enable seamless data flow across platforms
- Continuous Training and Change Management
- Embed AI education into clinical training
- Provide ongoing support to reduce technostress
- Balanced Automation Strategy
- Automate routine tasks, not clinical judgment
- Maintain human oversight in decision-making
- Data-Driven Workforce Planning
- Use predictive analytics for staffing optimization
- Align AI deployment with healthcare staff retention strategies
Conclusion: From Burnout Mitigation to Workforce Reinvention
The intersection of Generative AI, automation in healthcare, and digital health transformation marks a pivotal shift in how healthcare systems approach workforce sustainability.
When implemented effectively, these technologies:
- Reduce administrative burden
- Enhance clinical decision-making
- Improve job satisfaction
- Strengthen retention
However, their success depends on execution. Poorly designed systems can intensify burnout, while well-integrated solutions can fundamentally redefine nursing practice.
The future of AI for nurses is not about replacing human care—it is about restoring it. By offloading repetitive and cognitive burdens, AI enables nurses to focus on what healthcare ultimately demands: human connection, clinical expertise, and compassionate care.
























.jpg)

.png)





















































_2.png)

















.jpg)